pain management & recovery
with Mari Hodges, Pain Coach & Alexander Techique Teacher
MScMed (Pain Management), TPS, M.AmSAT

I believe in the possibility of overcoming pain.
Overcoming pain means learning to take back control of life from pain and fear. For some people this may mean recovery from persistent pain and for others, the ability to live a fulfilling life despite pain while managing a chronic condition.
The nervous system is always changing. That gives us hope that pain does not need to be stuck forever[1]. Pain is influenced by the interaction of many aspects of life, including the body, reactions to pain, thoughts, beliefs, expectations, emotions and our surroundings, like relationships, culture, healthcare system and more. That also means that there are many “ways in” to change pain. Together we can change the conditions that impact pain[2].
I believe that living with pain is not inevitable with age. There is much we can do to prevent and reduce pain. Everyone’s pain experience is unique, and the conditions and contributing factors can be more or less modifiable. I believe that with practice, we can have more control over the way we are being, as we do what we choose to do in the way we choose to do it—to a greater and greater extent. With this practice, pain that has interfered with life takes a back seat (or goes away) and no longer controls life. With this practice, we can gradually recover aspects of life that were lost to pain.
An upward spiral
While pain and disability can lead us into a downward spiral of withdrawal from activity, negative mood and increasing pain, this process of empowerment takes us upward and outward. Life circles us around to revisit challenges, but we can begin to experience them differently. By continuously developing skills of nonjudgemental observation, nondoing and intention, we develop the ability to view life situations from new perspectives, ultimately becoming empowered to change our own experience.

Click image to enlarge
My role
My role in your pain journey is educator, guide, coach and fellow explorer. I do not aim to “fix” anyone’s pain. I believe in helping individuals initiate and travel along a journey toward greater health, well-being and personal transformation by inspiring and encouraging learning, curiosity and self-awareness. My help for others is founded in my own practice of this same approach and my continuing studies in pain science and rehabilitation. I guide clients toward self-discovery of self-acceptance, the experience of safety within themselves, joy of moving in new ways and increased confidence in their own ability to consciously choose courses of action despite, or free of, pain.
What I do
I take an approach based on the wholeness of the individual, including mind and body in an inseparable unity[3]. Every encounter is different and I aim to be present to your current conditions without preconceived assumptions.
I begin with listening to your story, seeking compassionately to uncover the multiple dimensions of your experience, conditions around the onset of pain and current pain, and the meaning of the pain for you. Everyone’s experience is different, and I take note of all the factors that contribute to your experience[4]. I create a safe space for you to explore the relationships among thoughts, feelings, behaviors, body and awareness.[5]
I’ll guide you through gentle exploration of movement and body organization while guiding your attention with my hands, words and/or images. I’ll demonstrate and help you to move in a smooth, organized and unhurried way. This will help you make self-discoveries of unhelpful habits and easier ways of moving, how you can reduce excess tension and effort, and how you can self-regulate to have greater choice in how you organize your body, move, think, react, feel and act. Throughout this practice I’ll encourage you to keep an expanded awareness of your self (body, movement, breath, thoughts, feelings), surrounding space and ground support. Our focus will be on how everything works as a whole, so we won’t prioritize any part over others; we’ll give attention to painful and nonpainful areas alike.
I’ll help you bring awareness to the different psychophysical protections at work, and in this safe process of exploration, we’ll experiment with letting them go. Together we’ll develop a practice of nondoing observation, intention setting and contemplative movement. We’ll practice stopping to reset and refresh, helping to instill your self-regulatory skills.
The discoveries you make will be the foundation for increasing your ability to move, think and attend to yourself differently, with reduced interference from these protections[5]. The process is one of continuous self-reflection, learning, and skills practice followed by further self-reflection.
With this mindful, integrated movement practice you are likely to experience greater wholeness, confidence and ease as your functioning improves, and this synergy helps to reduce pain. I’ll encourage you to include the physical movement practice that you learn in everyday life, so that you can have greater choice in the what and the how of everyday actions. This leads to a greater sense of calm and control[5]. Also importantly, the process helps you to reduce reliance on passive therapies that only alleviate pain short-term while developing lifelong self-care skills.
Throughout our encounters, I’ll share information about the amazing bodily protection system and ways you can turn down pain and other excess protections. I’ll encourage you to learn more about yourself and about pain, to cultivate curiosity around what is going on and to develop your ability to notice what you are doing. This practice nourishes an ever-evolving process of learning and self-reflection that includes movement, thoughts, emotions, attention and the body in an integrated way. This further empowers you to continue developing healthy physical and mental processes as well as greater freedom of choice.
An example
Kathy (not a real client, she is made up of a combination of common features of clients) came to me with neck pain that persisted following a car accident some years ago. She’d tried various therapies and medical treatments that gave her short-term relief, but the pain always came back and was causing her grief because of movement restrictions, lack of energy, depressed mood and relationship problems as well as anxiety and fear about her future. She thought that improving her posture might reduce the pain.
As we worked together, Kathy discovered that the pain’s persistence wasn’t exclusively related to her neck. She realized that she didn’t need to “fix” her posture, but that she could change the way she organized and used her body in sitting at her computer, driving, standing, moving and lying down. Hands-on work and use of imagery that felt right to her supported her in discovering patterns of tension and thought that were exacerbating her pain. As we explored attending to her whole self (including her whole body’s organization, space and support) before, during and after everyday movements, she experienced revelations around the relationships between her thoughts, feelings and subtle body reactions. She found that her growing ability to discern how she was performing these activities and her increasing ability to change made her more confident and less afraid to move. She gradually started back with the exercise classes and hiking she used to enjoy so much, and found that exercising and socializing now made her feel better instead of worse. She discovered triggers of pain episodes that included stress from work or family conflicts, negative thoughts about the future, and overdoing activity without appropriate rest. She gradually developed skills to address these contributing factors, as well as the knowledge, skills and preparation to ride out a pain episode without letting it spiral her down into despair again. A process of hard work on her part has enabled her to actually reduce pain, to keep her perspective during occasional pain flare-ups and to appreciate the process in and of itself as a means of ongoing personal transformation and growth.
My values
The values that imbue my practice are also the values that I seek to embody and to encourage in my clients. The combination of lifelong learning, cultivation of compassionate curiosity and continued development of self-awareness underlie the process I use for myself and in my practice helping people with persistent pain. The diagram below illustrates how learning, self-reflection and skill development work together in a continuous cycle, within an environment of safe exploration, to move from chronic pain and disability to self-empowerment.
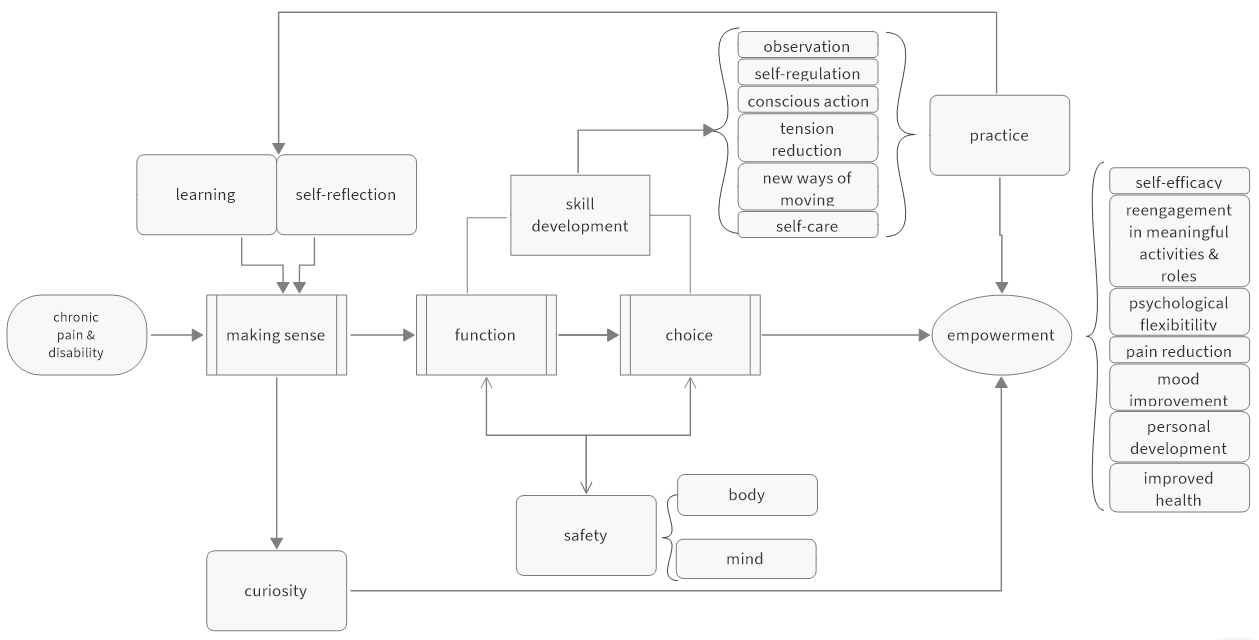
Definitions: self-regulation: ability to recognize and manage reactions to thoughts, feelings and happenings; self-efficacy: belief in one’s own ability to perform activities despite pain, which influences pain-related outcomes[6, 7]; psychological flexibility: ability to persist in or change behavior as a conscious response to thoughts, feelings, situations and personal goals and values[8].
My curiosity and desire to learn about pain and recovery from pain fueled my initial solo forays into the world of pain science and further advanced study. I discovered that my own fascination with the science of pain helped me to make sense of my own pain and to help other make sense of theirs[5]. I love to share what I learn with clients—even those who do not have persistent pain. It is inspiring to me to hear clients’ reflections on their own pain experiences and how these experiences are different from what they would have been because they have a better understanding and reduced sense of threat. This is my motivation: empowering others to transform their own lives and live better through learning, curiosity and self-reflection.
Access to pain management for all
Inspiring learning, curiosity and self-reflection is also a way to make self-management of pain more available to all. Active engagement in self-management is fundamental to positive change in pain and functioning[4, 9]. While individuals with persistent pain may tend to reduce and restrict activity—often influenced by their well-intentioned healthcare professionals[10, 11]—acquiring psychophysical skills of self-management can enable them to maintain involvement in meaningful activities, increase confidence and discover ways of moving that not only don’t hurt, but also contribute to well-being.
References:
- Siddall, P.J., Neuroplasticity and pain: what does it all mean? Med J Aust, 2013. 198(4): p. 177-8.
- Turk, D. and E. Monarch, Biopsychosocial Perspective on Chronic Pain, in Psychological Approaches to Pain Management: A Practitioner’s Handbook, Third Edition, D.C. Turk and R.J. Gatchel, Editors. 2018, Guilford Publications.
- Alexander, F.M., Use of the Self. 1932, London: Integral Press.
- Linton, S. and M. Nicholas, After assessment, then what? Integrating findings for successful case formulation and treatment tailoring, in Clinical pain management: practice and procedures, H. Breivik, et al., Editors. 2008, Hodder Education Group: London.
- Caneiro, J.P., et al., From Fear to Safety: A Roadmap to Recovery From Musculoskeletal Pain. Phys Ther, 2022. 102(2).
- Asghari, A. and M.K. Nicholas, Pain self-efficacy beliefs and pain behaviour. A prospective study. Pain, 2001. 94: p. 85-100.
- Jackson, T., et al., Self-efficacy and chronic pain outcomes: a meta-analytic review. J Pain, 2014. 15(8): p. 800-14.
- McCracken, L.M. and S. Morley, The psychological flexibility model: a basis for integration and progress in psychological approaches to chronic pain management. J Pain, 2014. 15(3): p. 221-34.
- Cosio, D. and E. Lin, Role of Active Versus Passive Complementary and Integrative Health Approaches in Pain Management. Glob Adv Health Med, 2018. 7: p. 2164956118768492.
- Ng, W., et al., Barriers and enablers influencing healthcare professionals’ adoption of a biopsychosocial approach to musculoskeletal pain: a systematic review and qualitative evidence synthesis. Pain, 2021. 162(8): p. 2154-2185.
- Darlow, B., et al., The association between health care professional attitudes and beliefs and the attitudes and beliefs, clinical management, and outcomes of patients with low back pain: a systematic review. Eur J Pain, 2012. 16(1): p. 3-17.
Read the article on modern pain science and how AT helps reduce pain co-written by colleague Tim Cacciatore, PhD, and me.
Check out my blog for tips on reducing pain, strain and anxiety and improving balance, ease of movement and well-being.
Memberships
Become a Member and Get Discounts on Classes
Group classes include Spring in Your Step!, an online dance movement class you can do at your own pace, in your own way. Check back or sign up for the newsletter to find out about upcoming group classes.

